Rheumatoid Arthritis

Described as a chronic auto immune disease, rheumatoid arthritis causes inflammation of the joints and tissues of the body. It may cause pain, swelling, stiffness and loss of function in your joints.
Rheumatoid arthritis can produce diffuse inflammation in the lungs, pericardium, pleura, sclera, and nodular lesions and in subcutaneous tissues under the skin. The symptoms of rheumatoid arthritis are recurring. In certain cases, it may lead to long-term joint damage, resulting in chronic pain, loss of function and disability. Rheumatoid arthritis affects approximately 1% of the adult population. It is found that more women than men are affected with rheumatoid arthritis.
Causes of rheumatoid arthritis
Though the exact cause of rheumatoid arthritis is
not clear, research indicates that rheumatoid arthritis might be the result of
bacterial, viral or fungal infection that triggers auto immune response. Other
possible factors that might contribute to the occurrence of rheumatoid
arthritis include heredity and hormones. Environmental factors like smoking
tobacco are also found to increase the risk of developing rheumatoid arthritis.
It is also said that rheumatoid is the result of autoimmunity. To understand autoimmunity, we need know the working of our immune system. The human immune system contains cells and proteins that fight infections. Auto immune disease is the result of failure in the immune system wherein it fails to recognize part of our body that is affected by virus and bacteria.
Though rheumatoid arthritis affects other tissues, the principal target is synovial membrane (synovium) that secrets synovial fluid to the joints. The fluid, also termed as joint fluid, lubricates and nourishes the joint. When the membrane is affected or destroyed, it becomes inflamed and can thicken and erode. As a result, the synovial fluid is also destroyed and is not secreted in the joints. In certain cases, the structures surrounding the joints also get affected thus leading to joint deformities.
Symptoms of rheumatoid arthritis
Rheumatoid arthritis is generally characterized by pain in one or many joints of the body. For instance, one can feel the pain as well as swelling both wrists. Hand joints like knuckle joints, and wrists, elbows, knees, ankles, feet and larger joints like shoulders, hips, and jaw are often affected by rheumatoid arthritis. People who suffer from the condition for many years might feel stiffness in the vertebrae of the neck.
Rheumatoid arthritis often occurs in a symmetrical pattern affecting different joints on both sides of the body. The general joint symptoms of rheumatoid arthritis include
-
Stiffness resulting in the inability to move the
joints. Some may feel the stiffness in the joints soon after they wake up that
does not subside for more than 30 minutes.
- Inflammation causing redness, tenderness and warmth in
the affected area/joint
- Swelling or puffiness around the affected joint
- Nodules or hard bumps might appear on or near the
joint, especially near the elbows.
- Pain because of inflammation or swelling of the joint.
Pain might also occur from working the joint too hard.
Other than joint symptoms, the normal symptoms associated with rheumatoid arthritis include the following
-
malaise
-
fever
-
fatigue
-
loss of appetite
-
weight loss
-
muscle aches and
-
weakness or loss of energy
Rheumatoid arthritis may also trigger the following condition in certain people.
-
Inflammation / dryness of the glands of the eyes and
mouth resulting in Sjogren's syndrome
-
Pleuritis, inflammation of the lung lining resulting in
chest pain with deep breathing, shortness of breath or coughing.
-
Nodule inflammation of the lungs
-
Pericardium, inflammation of the tissue surrounding the
heart called pericarditis. This can cause chest pain that changes in intensity when
lying down or leaning forward.
-
Anemia, decreased number of red blood cells
-
Felty's syndrome that appears because of decrease in
the white blood cells.
-
Tiny black areas around the nail beds or leg ulcers
resulting in vasculitis, a very rare condition that impairs blood supply to
tissues and leads to tissue death (necrosis).
Diagnosis
There is no single proven method to diagnose
rheumatoid arthritis. The physician performs a variety of tests to confirm that
you have rheumatoid arthritis and plans for a treatment accordingly. This might
include all or any one of the following
Medical History : The doctor checks whether you have history of joint aches, or joint stiffness. This might be done through a Health Assessment Questionnaire (HAQ) and the Arthritis Impact Measurement Scales (AIMS).
Physical Exam : The physician might perform physical examination like checking the joints for swelling or tenderness, motion of the joints, and mal alignment of the joints. He/She might also check for symptoms in other organs like skin, lungs, and eyes.
Lab Tests : Lab test is prescribed in cases where the diagnosis becomes difficult through physical examination. These tests might include complete blood count test, Erythrocyte Sedimentation Rate (ESD or sed rate), C-Reactive Protein, Rheumatoid Factor, and Antinuclear antibodies (ANA).
Imaging Studies : Imaging studies including X-rays, Magnetic Resonance Imaging (MRI), Joint Ultrasound, and Bone Densitometry (DEXA) might also be prescribed to diagnose the presence of rheumatoid arthritis.
Treatment of rheumatoid arthritis
There is no cure for rheumatoid arthritis.
However, the symptoms or the pain could be alleviated through several methods
including medications and exercises. It is ideal to meet a doctor soon as you develop
any of the above said symptoms.
Diet is found to be an effective treatment for rheumatoid arthritis. Your physician might advise you to partake of foods consisting of omega-3 fatty acids. Being overweight marks the entry point for any condition; rheumatoid arthritis being exception. Your doctor might prescribe you to lose weight, so that the pains and stiffness in the joints could be decreased. The other treatment includes exercise and rest. Regular cardiovascular exercise like swimming bicycling, stretching can alleviate your joint pains.
Occupational therapy and physical therapy are also found to be somewhat effective in treating rheumatoid arthritis. Occupational therapies include exercises to the commonly affected areas like wrists, fingers, and joints. This might include education of body biomechanics, use of splints like hand splints and wrist splints. Your physician might sketch out a structured program upon the diagnosis of your symptoms.
The best way to alleviate pains or swelling in the joints would be to use ice, heat, massage, ultrasound, warm wax and electric stimulation around the affected areas. However, consult your physician before performing the same.
Oral medications like non-steroidal anti-inflammatory drugs (NSAIDs) such as aspirin, ibuprofen, naproxen, and etodolac are commonly prescribed for treating rheumatoid arthritis. These medications are at times combined with sucralfate and misoprostol or proton pump inhibitors like omeprazole or pantoprazole, since NSAIDs might cause some stomach problems. Steroids either in oral form or injection are also recommended for the treatment of rheumatoid arthritis.
DMARDS or disease-modifying anti-rheumatic drugs including hydroxycholoquine, sulfasalzine, methotrexate, D-penicillamine, gold salts, azathioprine, and cyclophosphamide are used as the second-line medications in treating rheumatoid arthritis. These are generally taken for months or years. Other medications prescribed for treating the condition include Methotrexate, D-penicillamine, and Anti-TNF alpha factor medications. Cortisone injections are also prescribed in treating symptomatic joints.
Surgery is the last option for rheumatoid arthritis and it is very rarely performed. The surgical options include either a total hip replacement, or total knee replacement, if the hip or knee is affected.
Top of the Page: Rheumatoid Arthritis
Tags:#rheumatoid arthritis #symptoms of rheumatoid arthritis #cause of rheumatoid arthritis #treatment of rheumatoid arthritis #
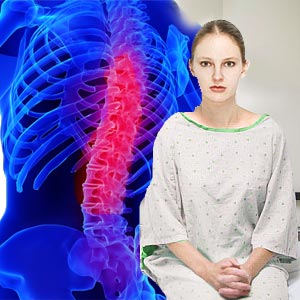 Slipped Disc
Slipped Disc Knee Replacement for Women
Rheumatoid Arthritis
Osteoarthritis
Drop Wrist Deformity
Ankylosing Spondylitis
Spinal Decompression
Scoliosis Treatment
Cause of Osteoporosis
Osteopenia
Bone Density Test
Disc Herniation
Tennis Elbow Symptoms
Restless Leg Syndrome Symptoms
Other health topics in TargetWoman Women Health section:
General Women Health

Women Health Tips - Women Health - key to understanding your health ...
Cardiac Care
Women's Heart Attack Symptoms - Identify heart problems...
Skin Diseases
Stress Hives - Red itchy spots ...
Women Disorders
Endocrine Disorder - Play a key role in overall wellbeing ...
Women's Reproductive Health
Testosterone Cream for Women - Hormone replacement option ...
Pregnancy
Pregnancy - Regulate your lifestyle to accommodate the needs of pregnancy ...
Head and Face
Sinus Infection - Nearly 1 of every 7 Americans suffer from ....
Women and Bone Care
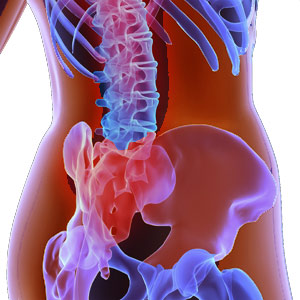
Slipped Disc - Prevent injury, reduce pain ...
Menstrual Disorders
Enlarged Uterus - Uterus larger than normal size ...
Female Urinary Problems
Bladder Problems in Women - Treatable and curable ...
Gastrointestinal Disorders
Causes of Stomach Ulcers - Burning feeling in the gut ...
Respiratory Disorders
Lung function Test - How well do you breathe ...
Sleep Management

Insomnia and Weight Gain - Sleep it off ...
Psychological Disorders in Women
Mood swings and women - Not going crazy ...
Supplements for Women
Women's Vitamins - Wellness needs...
Natural Remedies

Natural Diuretic - Flush out toxins ...
Alternative Therapy
Acupuncture Point - Feel the pins and needles ...
Women Health Directory
Top of the Page: Rheumatoid Arthritis
Popularity Index: 100,512

