Breast Calcification
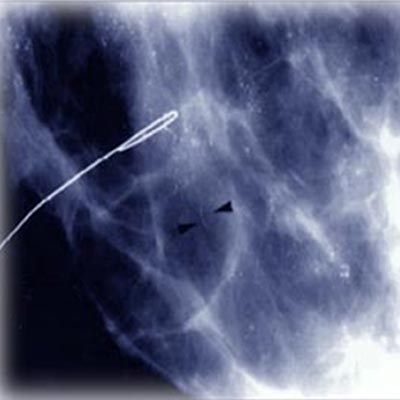
Calcification is a common process where small spots of calcium spots deposit themselves in breast tissue. These deposits can be the result of aging or other breast conditions such as fibroadenomas or cysts. Inflammation or foreign bodies such as implants or stitches can also lead to calcification.
Calcium phosphate crystals tend to aggregate into clumps, more so in collaboration with collagens. Collagens are insoluble proteins found in tissues. Calcification can occur in tissues and muscles of the hips, shoulders, elbows, hands and chest also.
Probable causes of breast calcifications
Injury or breast surgery can lead to microcalcification. Surgery such as silicone implants or removal of tissues are other probable causes. If you have undergone radiation treatment in the chest area, you are at higher risk for developing breast calcifications. Calcium deposits within the milk ducts or within the breast arteries are other causes for developing breast calcifications. Any breast infection such as mastitis or dermatitis is yet another cause for calcification within the breast. Calcium deposit within the fluid of a benign cyst can also occur. Calcification can also occur in a benign growth such as fibroadenoma. Breast calcifications are not caused due to dietary calcium.
Types of Breast Calcification
Macrocalcifications: These are coarse calcium deposits and are usually representative of degeneration of the breasts, either due to inflammation, injuries or aging of the breast arteries. Such calcifications are generally benign and are usually found in women over the age of 50. They appear as large white dots or dashes on the mammogram. Macrocalcifications in the breast appear as calcium deposits in cysts or milk ducts.
Breast Microcalcifications
This type of calcification is found as tiny specks of calcium in the breast. A cluster is an area where there is a proliferation of many microcalcifications. Such clusters may be cancerous. Breast microcalcifications are not felt on self breast examination. When a mammogram shows a spot of calcium buildup, it is called a microcalcification.
By itself, microcalcification is not a cause for worry as it can occur due to many reasons, not always cancerous. It is when these microcalcifications in the breast appear in tight clusters of irregular shapes that they become cause for concern.
When these breast microcalcifications appear in a scattered manner, they are usually indicative of benign breast tissue. Biopsy of some tissue is done for diagnosis. Microcalcifications in the breast are common during menopause.
Breast calcification and mammogram
Such calcium deposits are so tiny and cannot be felt by you or your doctor. A mammogram is used to detect calcifications. The radiologist examines the shape, size and pattern of the calcifications to make a diagnosis. Sometimes, a biopsy is required to confirm the diagnosis. Since a mammogram reveals just an area of abnormal tissue, a stereotactic biopsy is used to locate the area to be biopsied. X rays are used to guide the radiologist.
Benign breast calcifications are dermal calcifications, milk of calcium calcifications, suture calcifications and lucent-centered calcifications. The Breast Image Reporting and Data System (BI-RADS) of the American College of Radiology (ACR) has categorized the types of calcifications. Calcifications can be grouped according to their distribution - segmental, regional, diffused, linear or clustered.
Lobular calcifications appear as uniform, sharply outlined and are most often punctuate or round. Lobular calcifications can often be mistaken for intraductal calcifications. They are usually benign. On the other hand, intraductal calcifications can appear in different sizes, density and form. Intraductal calcifications occur within the intraductal lumen and exhibit fine branching distribution. They are usually higher on the possible malignancy scale.
The best diagnostic tool to detect breast calcification is a high quality mammography done by a radiologist who is skilled in the proper positioning and compression of the breast. Such mammograms are best viewed on high-luminance viewers where extraneous glare and light is eliminated. The morphology is an important determinant in detecting malignancy of breast calcifications. A biopsy can confirm the readings.
When instances of calcification are detected, mammograms are routinely taken to determine the stability of the calcifications. Suspicious mammograms must be followed by core needle biopsy, as it is minimally traumatic and relatively less expensive than surgical biopsy.
A mammogram can pick up microscopic deposits of calcium within breast tissue or even tiny blood vessels. In about 15% of the cases, these clusters are malignant. As compared with a surgical biopsy where the surgeon uses a scalpel to remove a chunk of tissue, core biopsy involves insertion of a large needle through the skin. This is usually aided by computers. But some types of conditions necessitate surgical biopsy, such as when the lesion is next to the chest wall and not easily visualized.
Top of the Page: Breast Calcification
Tags:#breast calcification #breast calcification biopsy #breast calcification clusters #breast tissue calcification #breast microcalcifications
Cancer Staging and Grading
Mammogram - Breast Xray
Breast Ultrasound
Breast MRI
Breast Augmentation
More on Breast cancer

Stress and Breast Cancer
Breast Density and Breast Cancer Risk
Lower your Breast Cancer Risk
Breast Cancer Myths
Mastitis
Breast Cancer Awareness
Preventing Breast Cancer
Breast Self Exam
Breast Cancer Chemotherapy Treatment
Palpable Breast Mass
Breast Cyst
Breast Cancer Symptoms
Breast Calcification
Breast Cancer Treatment
Mastectomy
Top of the Page: Breast Calcification
Popularity Index: 101,478

