Uterine Prolapse
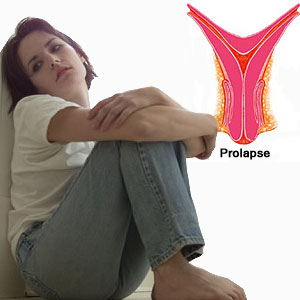
Uterine Prolapse is also referred to as pelvic floor hernia or pelvic relaxation. When uterus descends into or beyond the vagina, it is called as Uterine Prolapse. It is more common in postmenopausal women who have delivered more than once vaginally. Uterine prolapse is common, and the possibility of developing the condition increases with age.
Fifty percent of women who have delivered babies vaginally suffer from some degree of uterine prolapse. Find out what are the possible causes of uterine prolapse. Read up on the recommended treatment options for uterine prolapse.
Uterine Prolapse
The pelvic floor in a normal woman supports the uterus and the bladder just above the vagina. When the pelvic
floor is affected due to various causes (We will cover the causes later) and becomes damaged, the supported Uterus or Bladder will sag into the Vagina. In some cases, it may even cause bulging through the Vaginal opening.
A sagging uterus is variously called as Uterine Prolapse, Pelvic Floor Hernia or Pudendal Hernia. A sagging bladder is called as Bladder Prolapse or Cystocele.
In other words, falling or sliding of the uterus from its usual position in the pelvic cavity into the vaginal canal is called uterine prolapse. In few cases the uterus slips and goes right into the vagina. In a mild case of uterine prolapse, the cervix protrudes into the lower part of the vagina in case of mild prolapse.
In moderate cases the cervix protrudes past the vaginal opening, in case of severe prolapse the entire uterus protrudes past the vaginal opening. Uterine prolapse is described based on the part of the uterus and vagina involved.
Cystocoele: Prolapse of the front wall of the vagina (right below the bladder).
Rectocoele: Prolapse of the back wall of the vagina (just in front of the bowel).
Proccidentia: Prolapse of the cervix beyond the entrance of the vagina.
Uterine prolapse in a woman could be entailed only to the vagina or to both the vagina and the uterus. To determine the exact level of uterine prolapse imaging tests such as MRI or ultrasound are used.
Causes for Uterine Prolapse
- Pelvic connective tissues and pubococcygeus muscles undergo trauma during childbirth, in particular while delivering large babies. Difficult labor and delivery also lead to muscle weakness. The tissues grow weaker and allow the uterus to slide down into the vaginal canal.
- With advancing age there is loss of muscle tone and muscle relaxation happens due to reduction of the female hormone estrogen. This condition can also lead to uterine prolapse.
- In rare cases pelvic tumor could be the cause.
- Women of Northern European origin are more prone to this condition when compared to women of Asian and African origin.
- Obese women are more likely to develop this condition as obesity causes additional strain on the pelvic muscles.
- Extensive coughing due to chronic bronchitis, Chronic Obstructive Pulmonary Disease (COPD) and asthma can lead to uterine prolapse.
- Excessive straining and pushing during bowel movements due to constipation can be a cause.
- Women with retrograde uterus are at higher risk for uterine prolapse.
Symptoms of Uterine Prolapse
Depending on the severity the symptoms for uterine prolapse vary. If the uterine prolapse is mild you might experience no symptoms at all. In case of moderate to severe uterine prolapse the most common prevalent symptoms are listed below:
- Feeling of heaviness in the pelvis
- Protrusion from the vaginal opening
- Low backache
- Pain during sexual intercourse
- A feeling of something falling out of the vagina.
- Repeated bladder infections.
- Excessive and abnormal vaginal discharge
- Difficulty in urinating which may lead to incontinence or urgency to urinate.
The symptoms are minimal in the morning; they worsen as the day proceeds and usually worsen towards the end of the day.
Treatment for uterine prolapse
Uterine prolapse is a progressive condition and worsens over time, if left untreated. There are various treatment options like surgical and non-surgical. Depending on the severity of the problem, your physician will suggest the right treatment for you. No treatment is required for mild vaginal prolapse. Listed below are the most often used treatment options.
Vaginal pessary: Uterine prolapse can be treated with the help of vaginal pessaries. These pessaries can be temporarily or permanently placed and are designed perfectly to hold the uterus right in place. They are available in various shapes and sizes, your physician will choose the right one for you. Vaginal pessaries have to be cleaned periodically by self, in case of irritation or foul smelling discharge your physician has to clean it.
Hormone therapy: Resorting to estrogen replacement may check further weakening of the tissues and muscles supporting the uterus. But this must be taken on medical advice.
Changes in lifestyle: If the patient is overweight, then the doctor will suggest some exercises and help the patient shed the extra weight. Doctor's advice on how to reduce weight and maintain it, they train the patient in pelvic muscle strengthening exercises such as Kegel exercises.
Sacral colpopexy: Usage of surgical mesh to support the uterus. In this type of treatment the uterus is not removed, only supportive treatment for the uterus is given.
Hysterectomy: In severe cases vaginal hysterectomy is done, during this surgery sagging urethra, bladder, vaginal walls or rectum can be corrected simultaneously.
Prevention of uterine prolapse
- Prenatal and postpartum Kegel exercises help in tightening the pelvic floor musculature. These exercises also help to strengthen the vaginal muscles and reduce the overall risk of developing uterine prolapse.
- For postmenopausal women estrogen replacement therapy is highly recommended. This will help them maintain their muscle tone including the pelvic muscles.
- Try and maintain a healthy weight, this will help prevent such conditions.
- Cut down on smoking if you have chronic bronchitis.
- Eat a healthy diet.
- Follow proper and correct lifting techniques, minimize lifting heavy things.
Top of the Page: Uterine Prolapse
Tags:#uterine prolapse

Enlarged Uterus
Bacterial Vaginosis
Yeast Infection
Irregular Menstrual Cycle
PMS - Menstruation
Dysmenorrhea
Hypomenorrhea
Mid Cycle Bleeding
Pelvic Organ Prolapse
Vaginal Atrophy
Cervix Cancer
Abnormal Pap Smear
Polycystic Ovarian Syndrome
Ovulation Pain
Uterine Prolapse
Fibroid Tumor
Menorrhagia
Endometriosis Symptom
Galactorrhea
Hysterectomy
Blocked Fallopian Tubes
Menopause and Weight Gain
Premature Menopause
Surgical Menopause
Other health topics in TargetWoman Women Health section:
General Women Health

Women Health Tips - Women Health - key to understanding your health ...
Cardiac Care
Women's Heart Attack Symptoms - Identify heart problems...
Skin Diseases
Stress Hives - Red itchy spots ...
Women Disorders
Endocrine Disorder - Play a key role in overall wellbeing ...
Women's Reproductive Health
Testosterone Cream for Women - Hormone replacement option ...
Pregnancy
Pregnancy - Regulate your lifestyle to accommodate the needs of pregnancy ...
Head and Face
Sinus Infection - Nearly 1 of every 7 Americans suffer from ....
Women and Bone Care
Slipped Disc - Prevent injury, reduce pain ...
Menstrual Disorders
Enlarged Uterus - Uterus larger than normal size ...
Female Urinary Problems
Bladder Problems in Women - Treatable and curable ...
Gastrointestinal Disorders
Causes of Stomach Ulcers - Burning feeling in the gut ...
Respiratory Disorders
Lung function Test - How well do you breathe ...
Sleep Management

Insomnia and Weight Gain - Sleep it off ...
Psychological Disorders in Women
Mood swings and women - Not going crazy ...
Supplements for Women
Women's Vitamins - Wellness needs...
Natural Remedies

Natural Diuretic - Flush out toxins ...
Alternative Therapy
Acupuncture Point - Feel the pins and needles ...
Top of the Page: Uterine Prolapse
Popularity Index: 102,403

